Cardiology
We navigate the high complexity of cardiology billing, from diagnostic tests and catheterizations to surgical procedures, ensuring precise coding and modifier use to capture the full value of your specialized services.
Native and cross-platform mobile solutions delivering intuitive user experiences, robust performance, and seamless integration with your existing systems.
Design and development of secure, scalable REST and GraphQL APIs with microservice architectures that enable faster releases and seamless integrations.
User-centered design combining research, usability testing, and modern visual design to create intuitive experiences aligned with your brand.
Manual and automated testing services covering functionality, security, performance, and regression for reliable software delivery.
End-to-end SaaS product development including multi-tenant architecture, subscription systems, usage analytics, and scalable cloud deployment.
Database architecture and data modeling services focused on normalized schema design, relationship mapping, and long-term maintainability.
Integrate SQL and NoSQL data stores with applications, APIs, and third-party systems to ensure reliable and secure data flow.
Design and implementation of multi-tenant systems with tenant isolation, role-based access controls, and scalable resource management.
Ongoing monitoring, performance optimization, security updates, and enhancements to keep your applications stable and future-ready.
Clear requirements, stakeholder alignment, and Agile execution through expert business analysis, Scrum practices, and continuous collaboration.
Strategic consulting covering legacy system modernization, cloud migration planning, architecture audits, and technology roadmaps.
Design and implement scalable, secure, and efficient IT architectures that support business growth and technological advancements.
Strategic consulting covering legacy system modernization, cloud migration planning, architecture audits, and technology roadmaps.
Strategic consulting covering legacy system modernization, cloud migration planning, architecture audits, and technology roadmaps.
Comprehensive security services including penetration testing, vulnerability assessments, zero-trust architecture, and continuous monitoring.
Application security assessments, secure architecture design, and compliance support to protect sensitive data and meet industry standards.
From the moment your patient enters the door to the moment you receive payment for services rendered, our dedicated medical billing services team is committed to supporting your growth by addressing and improving key areas of your revenue cycle. Pameric RCM Plus oversees the entire revenue cycle to deliver risk-free cash flow through strict compliance and disciplined execution. By enforcing accuracy and regulatory alignment at every stage, we protect revenue, eliminate leakage, and convert earned care into collected revenue, consistently and without operational disruption.
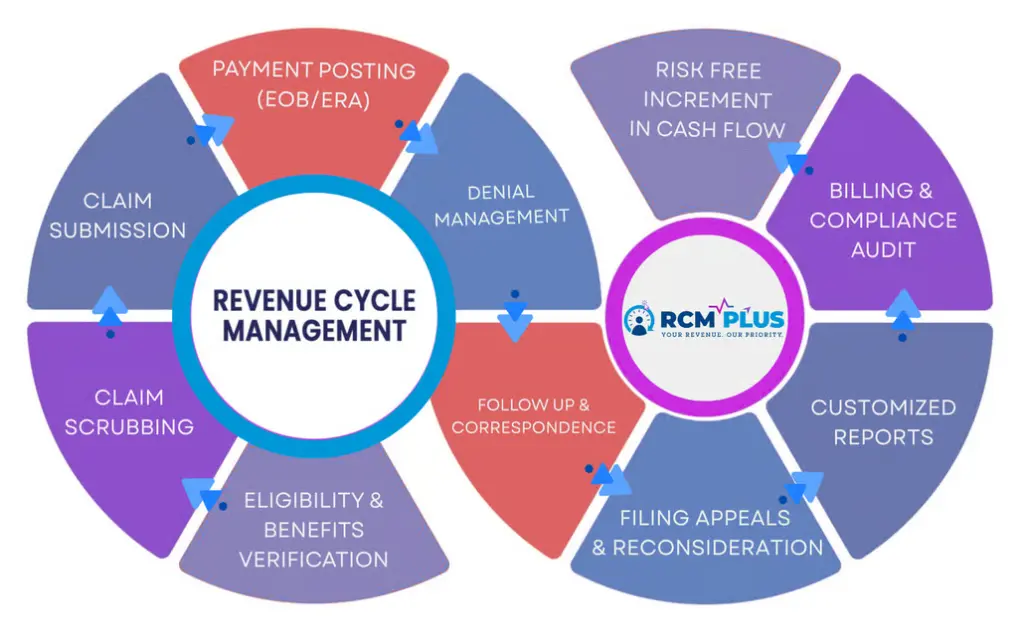
At Pameric RCM Plus, medical billing is not just claim submission. It is a controlled, compliance-driven revenue process designed to maximize collections while minimizing denials, delays, and audit risk. Our billing model covers the entire revenue cycle, from charge entry to final payment resolution.
At Pameric RCM Plus, medical billing audits are designed to do more than identify errors. Our audits are structured to reduce risk, protect revenue, and strengthen long-term compliance by examining every critical point in the revenue cycle.
At Pameric RCM Plus, quality is not just a buzzword. It is the foundation of our billing work and the reason providers trust us. Quality means accuracy, reliability, insight, and accountability at every step of the revenue cycle.
We ensure accurate patient demographics, proper CPT, HCPCS, and ICD coding, and complete documentation so claims are accepted the first time.
From verifying insurance eligibility before service to final payment posting and denial follow-up, our team follows standardized quality checkpoints. This reduces errors and improves cash flow.
Even small mistakes such as a wrong date of birth or incorrect modifier can trigger costly denials. That is why we apply multi-level reviews before submission.
When issues arise, such as denials or payer mismatches, we do more than resubmit claims. We analyze root causes, correct underlying workflows, and refine quality controls so the same issues do not repeat.
This is how quality becomes measurable and improves over time.
At Pameric RCM Plus, HIPAA compliance is not a checkbox. It is a daily operational discipline. One data breach, careless access, or unsecured transmission can expose providers to financial penalties, legal risk, and reputational damage.
That is why HIPAA compliance is embedded into how our team works, communicates, accesses data, and resolves issues. Compliance is never treated as an afterthought.
US healthcare providers are facing increased HIPAA enforcement and tighter scrutiny on outsourced billing operations. The biggest concerns we see in the market:
Our operating model is built specifically to address these risks.
We operate on one principle: If it cannot be audited, it is not compliant.
That is why Pameric RCM Plus focuses on controlled access, traceability, and disciplined processes so providers stay protected even as scrutiny increases.
At Pameric RCM Plus, we understand that superior revenue cycle management requires deep specialty-specific knowledge. Each area of medicine has unique coding, documentation, and payer rules. Our team does not just process claims; we become experts in your field to protect your revenue and ensure compliance.
We navigate the high complexity of cardiology billing, from diagnostic tests and catheterizations to surgical procedures, ensuring precise coding and modifier use to capture the full value of your specialized services.

We expertly manage the broad range of E/M codes, chronic care management, and annual wellness visits, ensuring accurate documentation and coding for both routine and complex patient encounters.

We handle the diverse coding needs of a family practice, from acute care and pediatric visits to chronic disease management in adults, ensuring accurate billing across all age groups and patient conditions.

We are proficient in the nuances of behavioral health billing, including E/M codes, psychotherapy integration, telepsychiatry services, and individual and group therapies, ensuring compliance and maximizing reimbursement.
We manage the intricate billing for nephrology services, including in-office consults, dialysis treatments, and ESRD-related care, with expert knowledge of capitated payment models.
We specialize in urology-specific CPT codes for surgical procedures, scopes, and cancer care, ensuring accurate billing and robust reimbursement for both office and facility-based services.
We optimize revenue for endoscopic procedures, colonoscopies, and related services, with expert knowledge in correct coding, modifier application (for example -51 and -59), and management of bundling issues.
We accurately code complex pulmonary services, including critical care, bronchoscopies, and sleep studies, ensuring full reimbursement for both diagnostic and therapeutic interventions.

We handle the full spectrum of OB/GYN billing, from routine wellness and global maternity packages to complex surgical procedures, ensuring accurate coding for both office and surgical services.
We navigate specialized billing for liver disease management, including complex diagnostic testing and treatment regimens, ensuring billing accuracy for this gastroenterology subspecialty.

We specialize in podiatry-specific CPT coding for surgical procedures, wound care, and orthotics, ensuring accurate billing and robust reimbursement for routine and surgical foot and ankle care.
We expertly bill infusion services, complex drug administration, and E/M visits central to rheumatology, ensuring proper reimbursement for both medication and management.
We efficiently manage high-volume procedures, biopsies, and lesion removals, ensuring accurate coding and maximizing reimbursement for medical and cosmetic dermatology services.

We handle immunology billing, including complex infusion services, allergy testing, and immunotherapy, ensuring ICD and CPT coding reflects the sophistication of care delivered.

We manage endocrinology billing for complex E/M visits, diabetes management, hormone therapies, and bone density studies.

We specialize in physical therapy billing, accurately coding units of time, modalities, and therapeutic procedures while maintaining compliance so you can focus on patient care.

We expertly code advanced wound care treatments, debridement, and hyperbaric oxygen therapy, ensuring documentation supports medical necessity for these specialized services.

We accurately handle well-child visits, immunizations, and pediatric-specific procedures, ensuring coding and billing reflects the unique care provided to younger patients.

We ensure precise coding for diagnostic and interventional radiology services, accurately applying modifiers and correctly billing technical and professional components.

We navigate complex coding for injections, nerve blocks, medication management, and trigger point injections, ensuring precise documentation and compliance for interventional and chronic pain reimbursement.

We manage billing for complex infectious disease care, including prolonged antibiotic therapies, consults, and specialized drug regimen billing.
Stop losing revenue to gaps in your workflow. Our add-on services are designed to eliminate bottlenecks, reduce denials, and accelerate your cash flow without increasing your internal workload.
Convert raw data into actionable dashboards, analytics, and custom reports aligned with business goals.
AI-powered automation, predictive analytics, and intelligent workflows that improve accuracy and operational speed.
Custom AI and machine learning models that enable forecasting, pattern detection, and smarter operational planning.
Automated build, deployment, and monitoring pipelines that increase release quality and delivery velocity.
Seamless integration of third-party and internal systems to enable secure data flow and process automation.
End-to-end cloud migration services covering assessment, rehosting, replatforming, and post-migration optimization.
Modernize legacy applications to improve performance, reduce technical debt, and extend long-term system value.
Cloud database administration services covering provisioning, monitoring, backup policies, security controls, and ongoing optimization.
Planned and validated migration of on-premise or legacy databases to cloud platforms with schema, data, and performance compatibility.